Author:Lv Han / Xu Hui / Zeng Na / Yin Hongxia / Liu Jiabao / Chen Jianghong / Wei Xuan / Zhao Lei Yang Zhenhan / Wang Zhencang
【Abstract】Objective To analyze the value of chest digital radiography (DR) in the initial diagnosis of secondary cases of COVID -19. Methods The radiological data from Beijing COVID -19 information and resource management platform “COVID-19 image database” were retrospectively analyzed. Twenty confirmed cases, including 14 males and 6 females (32-80 years old, mean 51.2±15.1 years old), who performed chest computed tomography (CT) scan and DR during his/her first visit to clinic were included. The interval times between CT and DR examination were from 1 to 53 hours, (mean 25.4±22.8 hours). According to the results of CT scan, the diagnostic ability of DR was analyzed. McNemar’s test was used to analyze the agreement between the diagnoses based on the CT and DR findings. Bland-Altman or Kappa analysis was used to analyze the consistency in number, distribution, and morphological features of the lesions identified on the CT and DR Results COVID-19 was identified in 19 of 20 cases by using CT (107 lesions), and 17 of 20 cases by using DR (54 lesions), respectively. The diagnostic accuracy of CT and DR was 95%, 85%, respectively. There was no statistical significance in diagnostic ability between DR and CT (P=0.5). For the determination of bilaterally distributed lesions, patterns of distribution among different lobes, diffused distribution and the morphological features of the lesions, the consistencies between the results of DR and CT were well (κ>0.6, respectively). The consistency between DR and CT is poor when recognizing multiple lesions(≥5). DR diagnosed two cases as normal, both presented as single pure ground glass opacity on CT, and the longest orthogonal diameters were 0.8 cm (≤1 cm) and 1.9 cm (1-3 cm). Conclusion Chest DR can be used to diagnose patients with COVID-19 if combined with the epidemic history. However, it is difficult for DR to identify single lesion with lower density in patients with mild symptom. A CT scan in time will provide additional information.
【Keywords】COVID-19; Tomography, X-ray computed; Digital radiography
Since the outbreak of COVID-19, the accurate identification of COVID-19 patients has been a clinical concern. Chest imaging examination is one of the most important diagnostic basis and plays an important role in clinical diagnosis and treatment. There have been many reports in the literature that indicated the CT features of first diagnosis of the confirmed cases, which provides a large amount of imaging information for accurate diagnosis of COVID-19. As a common imaging examination, chest X-ray also played an indispensable role, but there are relatively few reports on the characteristics of COVID-19 chest x-ray examination, and it only focuses on the review and analysis of severe and critical patients, which makes it lack the research of first diagnosis. Compared with CT examination, chest x-ray examination can greatly reduce the radiation and accurately detect COVID-19 patients in time. It can avoid the high requirement, long scanning time and corresponding human resource of CT equipment. Therefore, in order to provide an important objective basis for optimizing the diagnosis process and resource allocation scheme, this study retrospectively analyzes COVID-19 patients’ first chest x-ray diagnosis.
1 Materials and methods
1.1 Object of Study
We retrospectively analyze the 1552 confirmed or suspected cases of COVID 19 patients from "New Coronary Pneumonia Imaging Special Database" from January 11 to March 26, 2020. The database is the Beijing new coronary pneumonia information and sample resource management platform which was jointly established by the Beijing Municipal Science and Technology Commission and the Beijing Minicipal Health Commission. Among them, there were 1,020 cases (65.7%) doing chest CT examination for first diagnosis, and 532 cases (34.3%) doing chest DR examination for first diagnosis. Refer to the new coronavirus pneumonia diagnosis and treatment plan issued by the National Health Commission (Trial Seventh Edition) [1] to formulate the inclusion criteria for this study: ①Beijing permanent residents, judged as a local second-generation case based on the epidemiological history; ②First in treatment and with chest CT and chest DR examination; ③Have a history of close epidemiological contact, or have respiratory symptoms such as fever and cough; ④ Confirmation of nucleic acid detection positive by 2 RT-PCR methods. Exclusion criteria: ① Incomplete imaging data; ② Chest CT or
the DR image quality is poor and cannot be used for patient analysis; ③ COVID-19 review patient. Eventually 20 cases of COVID-19 patients from 9 hospitals are included, among them, 15 cases (75.0%) had DR examination for the first diagnosis, and 5 cases (25%) had CT examination for the first diagnosis. The patients are 14 males and 6 females, aged from 32 to 80 years, with an average age of (51.2±15.1) years, and 18 cases are normal type, 2 cases are heavy type. The interval between chest CT and DR examinations was 1h to 53 h, with an average interval of (25.4±22.8) h. The study was approved by the Ethics Committee of Beijing Friendship Hospital, Capital Medical University.
1.2 Inspection method
The CT and DR equipment adopt the corresponding parameters according to different hospitals that the patients went to. The inspection plan and results are in line with the corresponding requirements of the Beijing Medical Image Quality Control and Improvement Center. DR examinations are all posterior anterior chest x-ray. As for CT scans, we use 16-slice and above spiral CT scanning equipment, the patient is in supine position, end-inspiratory scanning, ranging from the tip to the bottom of the lung; the tube voltage is 120 kV, the tube current is automatically adjusted, and the collimator width is 64×0.6 mm or 128× 0.6 mm, lung window reconstruction (window width 1 600HU, window level -500HU), reconstruction layer thickness 1.0~2.0mm, layer spacing 1.0~2.0 mm, matrix 512×512.
1.3 Image Analysis
Three senior radiologists (with 8 to 10 years of experience in chest imaging diagnosis) read images individually on the multi-planar recombination images. If they disagree, they will reach an agreement after negotiation. Using CT examination results as the standard, the accuracy of DR diagnosis and lesion recognition rate were calculated. The following features in CT and DR images were counted separately: ①The location of the lesion, unilateral/bilateral, upper field/middle field/lower field (CT’s division on the coronal image based on DR standard); ②Characteristics of lesion distribution (whether it is diffuse, which means multiple lesions involving more than 2 lung fields); ③The location of the lesion (peripheral / central); ④ Form (quasi-circular/large flakes/strip flakes/linear/grid-shaped); ⑤The number of detected lesions is not counted if the lesions are diffusely distributed and connected into a sheet and cannot clearly distinguish the boundaries of the lesions.
1.4 Statistical analysis
Use SPSS 23.0 and R 3.6.3 software for statistical analysis. Counting data are represented by examples (%); measurement data conforming to normal distribution are represented by mean ± standard deviation (x±s), and measurement data not conforming to normal distribution are represented by median (interquartile range). The McNemar’s test was used to compare the diagnosis results of the two inspections, and the Bland-Altman test or Kappa test was used to evaluate the consistency of the number of lesions and the diagnosis of lesion features by the two inspection methods. P<0.05 is considered statistically significant.
2. Results
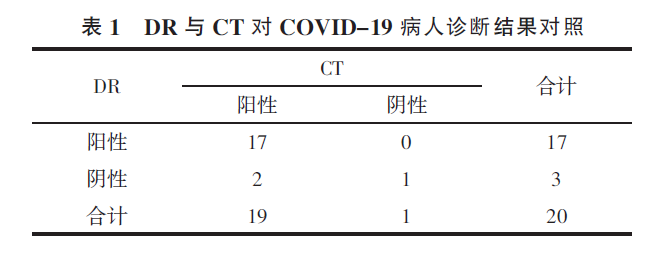
2.1 Comparing the diagnosis results of the two examinations, a total of 107 lesions in 19 patients were found in the CT examination, and no lesion was found in 1 case. A total of 54 lesions in 17 patients were found in the DR examination, and 3 cases were not detected. The CT’s detection rate was 95%, and the DR was 85% (Table 1). There was no significant difference in the diagnosis results of the two tests (P=0.5).
Table 1 Comparison of DR and CT diagnosis in COVID-19 patients
2.2 The consistency analysis of the number of lesions detected by the two inspections was based on CT as the diagnostic standard. The detection rate of the number of lesions by DR was 50.5% (54/107). The mean [95% confidence interval (CI)] of the difference in the number of lesions identified by DR and CT is 3.31 (95% CI: -9.42~16.05), and 1 value (6.25%) exceeds this range. The 93.75% value ‘s consistency is within the acceptable range (Figure 1). When the number of lesions is less than 5, the diagnosis consistency of DR and CT is acceptable; With the increase in the number of lesions (≥5), the diagnosis difference between the two examinations also increases, and DR has a poor judgment on the number of lesions.
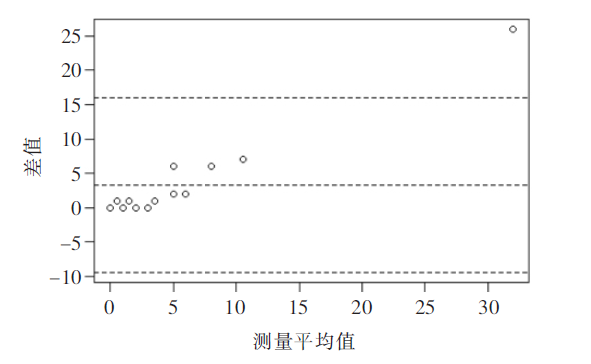
Figure 1 Bland-Altman figure for consistency test of the number of lesions
2.3 Consistency analysis of two examinations on the characteristics of the lesion
The analysis of the characteristics of the lesions by the two examinations showed that the diagnosis consistency of bilateral lesions, lung field distribution, diffuse distribution and morphology was good (both κ>0.6). See Table 2.
Table 2 Analysis and comparison of the characteristics of the patient’s lesions by the two examinations

2.4 Analysis of image features by 2 inspections
In 2 patients, the diagnosis results of the two examinations were inconsistent (Figures 2 and 3), DR was negative, but single lesions were seen on CT, which were round (1) and flaky (1) pure ground glass density shadows, the longest diameters of the two lesions were 0.8 cm (≤1 cm) and 1.9 cm (1-3 cm), and the volumes were 0.3 cm3 and 4.0 cm3. There were 18 patients with the same diagnosis of the two examinations (Figure 4). Most of the lesions were distributed under the pleura or along the bronchus. The longest diameter of the lesions was mostly 1~3 cm (64), and the next was not more than 1 cm (32 ), longer than 3 cm(11) is the least. The median volume of pulmonary involvement was 161.0 (16.2, 102.5) cm3, with patchy, round-like ground-glass opacity.
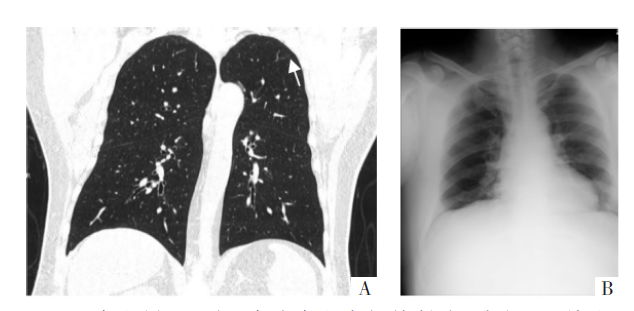
Figure 2 The patient was a 44-year-old male with a history of close contact with the confirmed patient. CT examination was performed first. The interval between the two examinations was 48 hours. Picture A is a CT image. There is a low-density round ground-glass density shadow (arrow) in the posterior segment of the left upper lobe tip, and the pulmonary involvement in the lung is 0.3 cm3; Picture B is a DR image, with no clear lesions. Considering that the density of the lesions is shallow and the lesions are small, so it cannot be displayed on the chest DR.

Figure 3 The patient was a 63-year-old male with a history of close contact with the confirmed patient. CT examination was performed first. The interval between the two examinations was 28 hours. Picture A is a CT image. There is a round ground glass density shadow (arrow) in the posterior part of the left upper lobe tip, and the pulmonary involvement is 4.0 cm3; Picture B is a DR image, with no clear lesions. Consider that the lesion was not displayed on the chest DR because the lesion was hidden by the ribs.
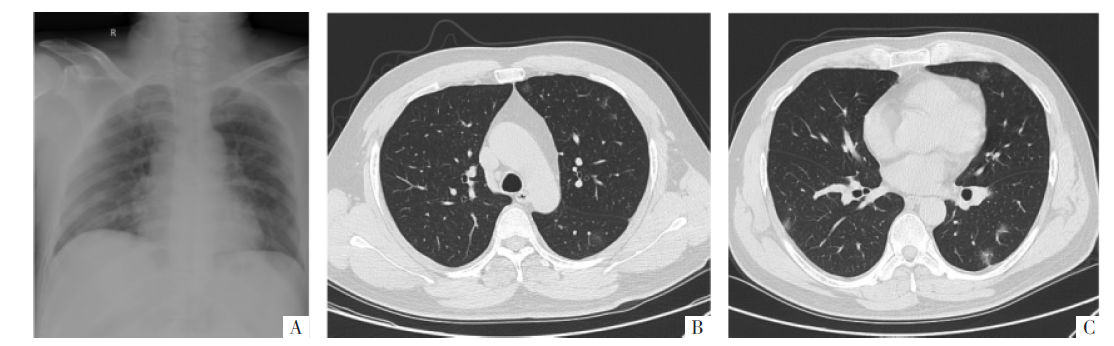
Figure 4 A 37-year-old male patient with a history of close contact with the confirmed patient. DR examination was performed first. The interval between the two examinations was 44 hours. Picture A is a DR image, pictures B and C are CT images. The diagnosis consistency of the two examinations is good, and multiple round-like lesions in both lungs can be seen
3. Discussion
At present, many documents have analyzed the chest CT characteristics of confirmed cases. It is common to have multiple lesions, involving one or both sides of the lung, and mainly focus on the lower lobe of the lungs or the lower lobe of the right lung. Most of the lesions are distributed under the pleura or along the bronchi, with patchy, round-like ground-glass density and so on, which are consistent with the pathological characteristics of viral pneumonia, and this study will not repeat them. This study aims to analyze the ability of imaging technology to judge the disease based on the number of clinically examined cases, rather than the detection rate of a certain lesion. Due to the multiple advantages of CT, such as high-density resolution, multi-planar reorganization, etc., the missed diagnosis rate is very low (about 2.3%) [4]; and its ability to detect lesions with lower density or smaller diameter is much higher than DR. For example, the 2 cases of DR reported in this study were negative but CT was positive. However, considering the current epidemic situation, under limited conditions, it is more important to accurately identify which patients are more likely to be suspicious cases and which can be ruled out, but not whether a lesion is considered COVID-19 lesion. Therefore, this study attempts to compare the recognition capabilities of different imaging examinations to provide a basis for optimizing the diagnosis and treatment process [5-6].
It is recognized in the industry that chest CT is more capable of detecting lung lesions than DR, and CT is recommended as the best imaging method for COVID-19 disease judgment [7]. However, in reality, not every hospital has the ability to do CT examinations for fever patients or suspected patients. Restricted conditions include, but are not limited to: ① No CT equipment in primary hospitals; ② No dedicated CT equipment for fever clinics, which cannot meet the requirements of inspection time, human resources configuration or site conditions to meet the needs of fever or suspected patients at any time; ③ Although with dedicated CT equipment , the number of patients with fever is too large to meet the demand. Therefore, in actual clinical work, there is still a considerable proportion of patients undergoing chest DR examination for the first diagnosis. In this study, 1 552 confirmed or suspected patients were reviewed, of which 34.3% (532/1 552) used DR in the first diagnosis; Among the 20 patients finally included, 75.0% (15/20) of the patients used DR in their first diagnosis. Therefore, it is necessary to attach great importance to the DR examination of COVID-19 patients.
In this study, the difference between DR and CT in diagnosing pneumonia was not statistically significant. The detection rate of CT in patients was 95%, and the DR was 85%, indicating that DR is not inferior to CT in disease judgment. On the one hand, because COVID-19 has the characteristics of multiple lesions and large patches of lesions, and the lesions are easier to be showed in DR examination; On the other hand, DR has good consistency with CT in judging the distribution characteristics, location, and shape of lesions, which further shows that DR has better disease judgment ability, so the application of chest X-ray examination in clinical diagnosis and treatment can achieve the examination purpose, especially for severe cases, due to the multiple and diffuse lung lesions, chest X-ray may have a better application effect [8]. Of course, DR has disadvantages in the accurate identification of lesions, especially in the detection and evaluation of small, low-density ground-glass density shadows (Figure 2), and lesions that are obscured by ribs and other structures (Figure 3). , the accuracy of judging the number of not less than 5 lesions is not good. In addition, this study included second-generation cases. It is possible that the virus has weakened its pathogenicity with the increase of transmission generation, making the lung lesions relatively few and small, which will further reduce the lesion detection ability of DR. Therefore, by adding lateral chest x-ray, using window technology to focus on observing suspicious areas, comparing the same part with the opposite side and adjacent parts of suspicious lesions, applying image inversion, local magnification and other technologies can further improve the diagnosis of diseases and the ability to recognize the number of lesions by chest x-ray.
Since Beijing does not clearly stipulate the first-diagnosis imaging examination method, nor does it stipulate the conditions for simultaneous application of chest DR and CT in a short period of time, this study is based on the analysis of the current practical imaging examinations to comprehensively evaluate the application value of chest x-ray. According to the new coronavirus pneumonia diagnosis and treatment plan (trial version 7) issued by the National Health Commission [1], chest imaging is an important clinical diagnosis basis for COVID-19, which can provide important clinical information, but it is not the only sources of diagnosis information or exclusion criteria, Therefore, in the process of diagnosis, especially for patients with mild symptoms, besides chest imaging, the diagnosis and treatment for patients should include medical history, symptoms and other perspectives. For example, the Beijing Friendship Hospital affiliated to Capital Medical University, a 3A hospital in Beijing where the author is located, before the formal application of shelter CT on March 9, 2020, the first diagnosis of fever patients was also chest DR, but No COVID-19 patient has been misdiagnosed or missed diagnosis. It can be seen that chest DR as a first-diagnosis imaging method does not affect the judgment of COVID-19 in actual work.
In summary, this study is based on the comprehensive evaluation of the application value of chest x-ray based on real events, chest DR examination can more accurately judge COVID-19 patients, and the overall clinical application effect is good. However, considering that some patients have few and small lesions, DR’s low resolution and no lateral chest x-ray and other factors will reduce the ability of chest DR to recognize the number of lesions. Therefore, when it is difficult to diagnose with only DR examination, chest CT examination can be performed in time if the conditions are available to further increase the diagnostic information. In view of the small number of patients included in this study and the limited representativeness, the conclusions of this study still need more rigorous experimental design and the support of large sample analysis results.
References
[1] Li Q, Guan X, Wu P, et al. Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia [J]. N Engl J Med, 2020.DOI:10.1056/NEJMoa2001316.
[2] Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China [J]. Lancet, 2020, 395: 497-506.
[3] Li K, Wu J, Wu F, et al. The clinical and chest CT features associated with severe and critical COVID-19 pneumonia [J]. Invest Radiol, 2020.DOI:10.1097/RLI.0000000000000672.
[4] General Office of the National Health Commission, Office of the State Administration of Traditional Chinese Medicine. Notice on Printing and Distributing the New Coronavirus Pneumonia Diagnosis and Treatment Plan (Trial Version 7) (Guoweiban Yihan [2020] No. 184) [EB/OL]. (2020 -03 -03) .http://www.nhc.gov.cn/
yzygj/s7653p/202003/46c9294a7dfe4cef80dc7f5912eb1989.shtml.
[5] Chung M, Adam B, Zhang N, et al. CT imaging features of 2019 novel coronavirus (2019-nCoV) [J/OL]. Radiology, 2020.DOI:10.1148/ radiol.2020200230.
[6] Xu X, Chen P, Wang J, et al. Evolution of the novel coronavirus from the ongoing Wuhan outbreak and modeling of its spike protein for risk of human transmission[J]. Sci China Life Sci, 2020, 63: 457-460.
[7] Chen N, Zhou M, Dong X, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study [J]. Lancet, 2020, 395: 507-513.
[8] Wang D, Hu B, Hu C, et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus -infected pneumonia in Wuhan, China[J/OL]. JAMA, 2020. DOI: 10.1001/jama.2020.1585.
[9] Adam B, Mei XY, Huang MQ ,et al. Chest CT findings in coronavirus disease-19 (COVID-19) relationship to duration of infection [J/OL]. Radiology, 2020. DOI:10.1148/radiol.2020200463.
[10] Liu Y, Yang Y, Zhang C, et al. Clinical and biochemical indexes from 2019-nCoV infected patients linked to viral loads and lung injury [J]. Sci China Life Sci, 2020, 63:364-374.
[11] Ai T, Yang ZL, Hou HY, et al. Correlation of chest CT and RT-PCR testing in coronavirus disease 2019 (COVID-19) in China: a report of 1014 cases[J/OL]. Radiology, 2020. DOI:10.1148/radiol.2020200642.
[12] Fang YC, Zhang HQ, Xie JC, et al. Sensitivity of chest CT for COVID -19: comparison to RT-PCR [J/OL]. Radiology, 2020.DOI:10.1148/radiol.2020200432.
[13] Lv Rong, Feng Yingyin, Zhang Yanan, et al. CT image characteristics and analysis of 17 cases of novel coronavirus pneumonia (COVID-19)[J].International Journal of Medical Radiology,2020,43:131-134.
[14] Tong He, Xu Yuanyuan, Yang Bo, et al. The diagnostic value of HRCT imaging of novel coronavirus pneumonia (COVID-19)[J].International Journal of Medical Radiology,2020,43:135-139.
[15] Ng MY, Lee EYP, Yang J, et al. Imaging profile of the COVID-19 infection: radiologic findings and literature review[J/OL]. Radiol Cardiothorac Imaging, 2020. DOI:10.1148/ryct.2020200034.
[16] Song FX, Shi NN, Shan F, et al. Emerging 2019 novel coronavirus (2019-nCoV) pneumonia [J/OL]. Radiology, 2020.DOI:10.1148/radiol.2020200274.
[17] Huang Lu, Han Rui, Yu Pengxin, et al. Correlation study of CT and clinical manifestations between different clinical types of novel coronavirus pneumonia [J/OL]. Chinese Journal of Radiology, 2020. DOI:10.3760/cma.j. issn.1005-1201.2020.0003.
[18] Xu Z, Shi L, Wang Y, et al. Pathological findings of COVID-19 associated with acute respiratory distress syndrome [J/OL]. Lancet Respir Med, 2020.DOI:10.1016/S2213-2600 (20)30076-X.
[19] Pan F, Ye T, Sun P, et al. Time course of lung changes on chest CT during recovery from 2019 novel coronavirus (COVID-19) pneumonia [J/OL]. Radiology, 2020. DOI:10.1148/ radiol.2020200370 .







